WHEN resources are scarce, priorities are set carefully to avoid compromising on necessities. That is a basic economic rule applicable to all spheres, including healthcare.
Recently, a controversy erupted in the Sindh caretaker government on the procurement of four robotic surgical systems at a hefty cost. Caretaker health minister Dr Saad Khalid Niaz was reported as saying, “I had halted the Rs4.247 billion deal for the procurement of four robotic surgery systems — one more for Jinnah Postgraduate Medical Centre, Karachi, two for Liaquat University Hospital in Hyderabad and one for the Gambat Institute of Medical Sciences. This annoyed the chief minister and those who are the beneficiaries of the procurement of robotic surgery systems.”
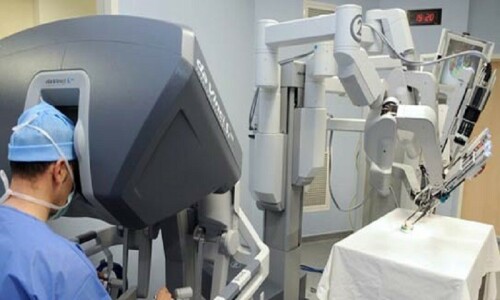
What is a robotic surgery system? Earlier, surgical interventions in the abdomen required cutting up the abdominal wall and involved long incisions, resulting in blood loss, post-operative pain, and the danger of infection. The advent of laparoscopic surgery largely overcame these issues.
During this minimally invasive procedure, surgeons enter the abdomen through a very small opening (hence the term ‘keyhole surgery’), with a camera attached to a flexible fibre-optic cable, which is linked to a monitor screen. Elongated instruments like scissors, forceps, etc, are passed through the opening and surgery is performed via the screen. Laparoscopic surgery has dramatically decreased recovery time as well as hospitalisation costs.
The first laparoscopic appendicectomy was performed in Germany in 1981. Today, it is considered a norm in various abdominal and thoracic surgeries.
As the application of digital technology advanced, so did the notion of robot-assisted surgery; a superlative of computer-assisted laparoscopic surgery. It is more accurate, precise, and less tiring for the surgeon.
It is indeed a marvel of science whereby computer-controlled robotic arms perform surgery. Sophisticated applications of memory devices and AI have even made remote surgery possible.
Cost of four robotic surgery systems equals a year of basic healthcare for 1.15m people in rural Sindh.
Despite its allure for surgeons, robotic surgery has been criticised in high-income countries for its prohibitive cost. Atul Gawande, an American author, surgeon, and current assistant administrator of USAID for global health, writes in his fascinating book, The Checklist Manifesto: How To Get Things Right: “Robots increased surgical costs massively and have so far improved results only modestly for a few operations, compared with standard laparoscopy.
Nonetheless, hospitals in the US and abroad have spent billions of dollars on them.“ The book is a story of the difficulties of developing and implementing a simple global Surgical Safety Checklist in operation theatres.
According to the 11th International Classification of Diseases (2019), there are currently 17,000 diseases, syndromes, and injuries. There are more than 6,000 generic medicines and over 4,000 medical and surgical procedures to deal with these afflictions, “each with different requirements, risks, and considerations”.
Healthcare systems pick and choose from this vast pool in accordance with their burden of disease, resources, and systems of prioritisation. Producers and suppliers of these medicines, instruments, devices, and equipment promote and push their products into healthcare systems, which later struggle to make appropriate choices between competing priorities and numerous pressures.
An unholy connivance between the two exists in almost every country, more pronouncedly in systems where internal checks and systems of prioritisation are weak or nonexistent.
In the case of medicines, for example, WHO realised the problem way back in 1977. It developed the concept of essential medicines. At that time, the WHO Model List of Essential Medicines contained 208 items.
The idea was that while many medicines are registered and available in the market, it is important to be selective, bearing in mind the medical needs of the majority of the population, in order to ensure the efficacy, safety, and cost-effectiveness of medicines. In keeping with this idea, WHO also maintains a list of priority medical devices.
In the case of health services, there is a quarter of a century of work done by the World Bank to prioritise the most-needed health services in low- and middle-income countries. This is now available in the form of a nine-volume study, the third version of Disease Control Priorities, available at dcp-3.org.
From thousands of health services, 218 priority health services have been shortlisted on the basis of their need and cost-effectiveness. L&MICs are urged to use this list to develop their own package of essential health services. Pakistan subsequently developed one.
Prioritisation in healthcare is a science. Health Technology Assessment agencies in high-income countries, and increasingly in middle-income countries, undertake extensive cost-effectiveness studies on new health technologies and interventions. They then give their verdict on the advantages in comparison to existing technologies and interventions and explain the cost.
Many a time, the cost is too high and the advantages are marginal. Therefore, policymakers decide not to spend the taxpayers’ money on procurement. The UK’s National Institute for Health and Care Excellence (NICE) is a great example of an HTA agency. It promotes evidence-based best practice and value for money.
How a country with 40 per cent stunted children — over 60pc in rural Sindh alone — can even think of abusing the taxpayers’ money on buying robotic surgical systems is beyond me.
At the federal level, we calculated that delivering an essential package of 88 highly prioritised essential health services to people at the primary healthcare level would cost $12.9 per capita per year. My back-of-the-envelope calculation shows that instead of buying four robotic surgical systems, Rs4.247bn can be used to provide a package of 88 highly prioritised essential health services to 1.15 million people for one year.
Dr Niaz has done absolutely the right thing in thwarting this procurement. There are already five robotic surgical systems that have been procured by the Sindh government, including two for a famous charity institute!
But how will the next minister decide? Without a scientific and institutionalised approach towards setting our priorities in publicly financed healthcare, we can only postpone such irresponsible procurements, not eliminate them.
The writer is a former SAPM on health, professor of health systems at Shifa Tameer-i-Millat University, WHO adviser on UHC, and member of the Pakistan Mental Health Coalition.
Published in Dawn, December 1st, 2023