18-year-old Sadia (all names have been changed) was brought into a clinic at a bustling tertiary care hospital by her father Noor Khan with high fever for the past three weeks.
She was diagnosed with typhoid and prescribed the standard oral antibiotics suitable to treat this disease.
The next week, Khan returned to the same clinic with his 20-year-old son Habib who had the same symptoms as his sister.
However, his condition was considerably worse and necessitated admission to hospital and intravenous antibiotics.
“Doctor sahiba, Habib has his exams in less than two weeks. Please fix him up soon,” Khan implored.
“We will try our best,” the doctor comforted him.
On the day of discharge, Khan walked into the clinic with heavy steps. Unable to see the doctor in the eyes, he said, “Doctor sahiba, the bill for the hospital admission is Rs 15,000. And the medicine that you have given now to be taken at home is also quite expensive. Can we do without this medicine?”
“If Habib is to get better, then this medicine is required,” the doctor replied.
“I know doctor sahiba, but this will be very difficult. I work in a local factory as a worker. I make Rs 15,000 per month. I have taken out a loan to pay for his treatment,” Khan said helplessly.
The doctor stepped in and arranged for part of his medical expenses to be waived by the hospital. Grateful as he was, Khan didn’t know that his ordeal was far from over.
Related: Superbug typhoid strain behind Pakistan outbreak
After a month, he was rushing his youngest child Mujeeb, 12, into emergency with high fever and convulsions.
“Since when has this been happening?” the doctor asked.
“For the past two weeks. We were giving him medicine from the local medical shop because well…” Khan replied.
“What!?” exclaimed the doctor
“Doctor sahiba, I didn’t have money to bring him to the hospital,” a dejected Khan stated, his eyes downcast.
Mujeeb was rushed to the Intensive Care Unit where he was treated with a number of very expensive intravenous antibiotics. His blood culture indicated multi-drug-resistant typhoid. He remained in the hospital for two weeks.
He was suffering, but so was his family who was now in massive debt. His elder brother Habib had left his studies to work in a motor repair shop to help pay for the household’s daily expenses.
Khan was facing problems at work because of taking leaves for his family’s illness. The mother, Bano Jee, was convinced that someone had done kala jaadoo (black magic) on her children.
Special report: The antibiotics resistance crisis: an emerging public health disaster
Unfortunately, for those within the medical profession, this story is not fiction — it represents a terrible reality, a classic example of how some infectious diseases, almost unheard of in the developed world, have not only lingered as major threats to our lives, but have actually gained in strength to wreak havoc on our populations.
This is evidenced by the fact that 40 per cent of the disease burden in Pakistan can be attributed to infectious diseases such as typhoid, tuberculosis and malaria.
Typhoid, a household term in our cities and villages, was relatively easy to treat up till recently. Two years back, multi-drug resistant typhoid was found within the localities of Hyderabad and Karachi.
According to reports, more than 800 cases of drug-resistant typhoid were found in Hyderabad alone in a 10-month period between 2016 and 2017.
This bug was sensitive to only two broad-spectrum antibiotics, the cost of which is exorbitant. Infectious disease specialists estimate the total treatment cost for 14 days to be roughly around Rs 50,000.
Broad-spectrum antibiotics are those that can kill a wide range of bugs; they are used when the bug is unknown, but these antibiotics increase resistance if used indiscriminately.
For someone who survives on daily wages, such treatment costs can put the entire household in financial catastrophe.
Read next: ‘Pakistan needs to know, tackle crisis resulting from antibiotic resistance’
What adds to the problem is that broad-spectrum antibiotics are unlikely to be found in small towns and shops, particularly in rural areas, where generic antibiotics availability ranges from 10 to 25 per cent.
Bacteria also know no boundaries — recently, the same bug was found in Swabi. The doctors in that locality reported that the patient was from Karachi.
A World Health Organization poster reads: “Our time with antibiotics is running out.” This is not a dramatic call for attention, but a tragic reality of the times that we live in.
The growing resistance among organisms to different antibiotics has developed and worsened over the course of decades due to our unfavourable systematic practices that lead to prescription of antibiotics, even when they are not medically indicated or required, such as in the case of viral infections.
Overuse of antibiotics is an increasing problem, as the recent Dawn editorial also suggests. This occurs due to the fact that patients themselves come to physicians looking for a quick fix, which they misconceive to be only through antibiotics, and demand to be prescribed antibiotics.
Alarmingly in our situation, it is easy to bypass physicians and just go to the corner store and buy any antibiotic we feel inclined to get, based on the advice of the storekeeper who may have no background even in pharmacy sciences.
A 2016 study from Peshawar demonstrated that 26 per cent of 800 respondents reported self-medication of antibiotics.

Another equally worrying factor is that many medical practitioners, amenable to the influence of pharmaceutical companies, prescribe these antibiotics in large quantities.
Such physicians accept favours and gifts — including simple office stationery, drug samples, trips to exotic destinations abroad among others — from pharmaceutical companies who, in exchange, require them to prescribe the more expensive antibiotics.
The complicity of these physicians, who are honour bound by their medical oath to put the interests of the patients above their own but fail do so, is another influencing factor within developing countries, including Pakistan.
Guidelines by the Pakistan Medical and Dental Council and the National Bioethics Committee on pharma-physician interactions exist but, to date, no physician has been held accountable or had his/her license revoked, although the practice is rampant. Since these guidelines have no teeth, it is hardly surprising that the practice continues to flourish.
Prevention works better than cure and is significantly cheaper in the long run also. This is even truer in cases of infectious diseases such as typhoid, tuberculosis, and dengue and so on.
Unhygienic food and drinking water and poor living conditions create a perfect milieu for infectious agents to thrive. The response of health authorities in such situations should not be reactive, but more efforts have to be geared towards primary prevention.
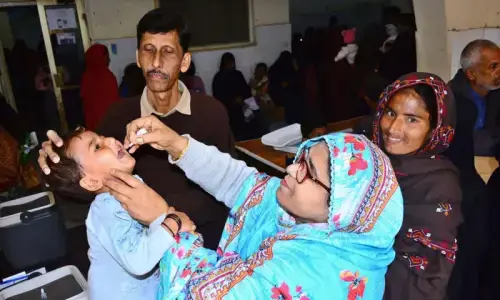
Preventive efforts include measures like vaccination, which is seriously neglected in Pakistan. A vaccination drive was conducted in Hyderabad recently only after cases of drug-resistant typhoid were found by a private university and the authorities duly alerted.
However, vaccination against the more common diseases in Pakistan should become part of the Expanded Program on Immunization (EPI), which itself faces a number of challenges, including limited resources and inadequate coverage.
General lack of awareness among public with respect to vaccination, along with limited effort by public health authorities, has relegated the importance of vaccination. These need to be revitalised in order to tackle this menace.
Also read: How Pakistan turned around its vaccination programme using technology
Serious efforts by the authorities to provide clean sanitation and provision of hygienic food should be done. With sewerage spilling over streets and vendors selling pakoras to eager buyers right next to a tertiary care hospital is a common site for all Pakistanis that does not even merit raising eyebrows.
While our chemists merrily dispense antibiotics to eager customers, our food stalls dispense fortified salmonella, the bacteria that causes typhoid. If we are serious in stopping infections short in their tracks, we need to get serious in preventing conditions that foster them.
The dangers of antimicrobial resistance are real with significant impacts. To combat this, the medical community has an essential role to play in limiting their prescriptions of antibiotics and raising awareness among public about dangers of self-medication and antibiotic overuse.
Health authorities also have to wake up from their restful slumber and focus their energies on preventive mechanisms as opposed to occasional stirrings when water is already under the bridge.
Are you a medical practitioner working on community and public health issues? Share your insights with us at blog@dawn.com