A woman dies while giving birth almost every hour in Pakistan, and many more never even reach that point, dying due to complications during pregnancy. The vast majority of these women are not being assisted by skilled health workers. This reality is even more worrisome in the province of Balochistan than in the rest of the country. Difficulties accessing healthcare facilities, a mixture of traditional customs and lack of awareness make the biggest but least populated Pakistani province a place where basic maternal health issues can develop into something very complex and often fatal.
Last year, 785 pregnant women out of 100,000 lost their lives in Balochistan. This rate is almost three times higher than the average in the whole of Pakistan. The reasons behind these appalling numbers are many: The province has some of the lowest national developmental indicators, a third of women marry before reaching the age of 15 and two thirds of women here are illiterate. Only three out of 10 pregnant women deliver their babies with skilled attendants present and less than a half of these mothers visit a health professional before their delivery. There has been little improvement in the last few decades.
The medical humanitarian organisation Doctors without Borders/Médecins Sans Frontières (MSF) runs maternal and paediatric healthcare programmes in four locations in Baluchistan (Quetta, Kuchlak, Chaman and Dera Murad Jamali), in cooperation with the local and provincial authorities. Some of the services offered are ante- and postnatal consultations, deliveries, referrals to specialised hospitals for any emergency or complicated deliveries, newborn care and resuscitation, breastfeeding promotion and nutritional support.
Last year, 785 pregnant women out of 100,000 lost their lives in Balochistan. This rate is almost three times higher than the average in the whole of Pakistan. The reasons behind these appalling numbers are many
Cultural differences across Balochistan don’t radically change the picture. MSF supported more than 8,000 deliveries in 2013, and provided just under 20,000 antenatal consultations. The majority of these free consultations were with pregnant women who were visiting an MSF clinic for the first time. In most cases, they did not return for a second visit and a significant number of patients did not give birth at the facility. Moreover, just a third of the women who delivered at such a clinic returned for a postnatal consultation. Patients and their families often prefer to have quick deliveries with the aid of drugs, usually administered by unskilled professionals. Once the baby is born they believe the job is done. But it is not.
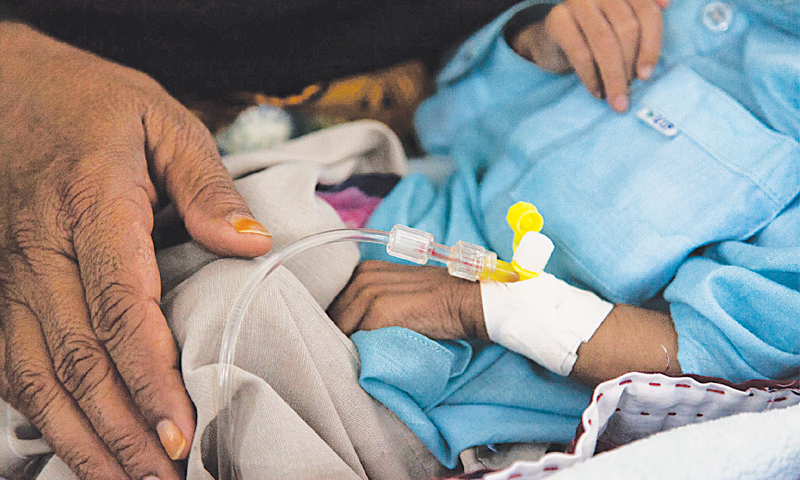 |
| A patient being attended to |
Doctor Cecilio Tan has been coordinating MSF’s medical projects in Balochistan province since early 2013. He explains some of the factors behind the high maternal mortality rates in the province and why maternal healthcare programmes should be a priority in Pakistan.
What is the state of the healthcare system in Balochistan?
In the cities there are tertiary hospitals (specialised) funded by the government, and private hospitals and clinics are mushrooming. These private establishments are expensive and are unaffordable for the average person living in the province. In the rural areas there may only be basic healthcare units, where patients are lucky if there is a nurse or a paramedic. A doctor or the necessary equipment may not be available
Why is the maternal mortality rate so high in this province?
Common factors are poverty and a poor literacy rate. There is also conflict and political instability in the province and the area is prone to natural disasters such as floods and earthquakes. Many people live in remote areas and women cannot access clinics for medical consultations. Moreover, the women’s nutritional health is worse than the men’s. On average, women in the province give birth to six to eight children and they very often have their first baby at the age of 16. Some women are underweight and when they become pregnant their health worsens.
What is the profile of the people who visit the healthcare facilities supported by MSF?
We assist populations from areas inhabited by different ethnic groups, as well as Afghans who cross the border seeking healthcare. Some of our patients are Afghan refugees, who settled in the area up to 20 years ago and so have essentially become part of the local community. We also see nomads, who spend the summer in Quetta and migrate to other places in winter. They are poor people and it is often difficult for our staff to communicate with them because they speak different dialects.
What are the main issues related to maternity in Balochistan?
One of the main ones is that most — eight out of 10 — women only attend the clinic once for antenatal care. This means our ability to offer follow-up care is limited. Most of the women deliver at home attended by non-trained relatives or neighbours. These unskilled birth attendants often use a medication for uterus contractions — available locally at a low price –— to make the births happen quicker. Wrongly administering this drug can lead to serious complications for both the mother and the newborn baby. In the worst cases, it can even lead to death. During emergency obstetric situations that may require further medical or surgical intervention, referrals to specialised hospital are sometimes hampered by the unavailability of male relatives to accompany the women. In this context a female patient is not allowed to travel without a male relative to accompany her, and the men (husband or other relatives) are usually busy working to support the family. The constraints posed by this are the reason why pregnant women often come to the clinic too late, when there is already a complication. It would be advisable that they visited the clinic several times during their pregnancy and for follow-up care after the birth, but this is not usually possible. If they are not at home, there is no one to look after the children, cook, fetch the water, etc. Another challenge is that there are not enough skilled female medics and health workers in the clinics and hospitals to treat the women.
What complications can happen during the birth if a trained delivery assistant is not present?
Complications can occur whether the birth is attended by trained personnel or not, but skilled staff present can save lives. There can be severe bleeding in the woman or the blood supply to the baby can be compromised. These crucial moments can really mean the difference between life and death for the mother and the baby. Skilled staff can recognise red flags and refer the patient to hospital as soon as possible, so the chances of survival increase.
As the women want to go home as soon as possible after the birth, they often choose to attend private clinics where the delivery is speeded up by injecting drugs such as oxytocin.
This can lead to severe complications for both the baby and the mother. In the facilities where we work we treat many babies who were born in private clinics and are in critical condition after having experienced a very stressful delivery.
What are MSF’s concerns after the birth?
We are trying to promote breastfeeding and highlight its importance, as sometimes babies are not given breast milk but honey, dark tea, etc. instead. This does not have nutritional value and affects their stomach. Cultural barriers make it complicated for mothers to breastfeed their babies. Many are responsible for a large household and often they already have a number of other children to care for.
Published in Dawn, Sunday Magazine, September 14th, 2014















































Dear visitor, the comments section is undergoing an overhaul and will return soon.