When people stop taking the new generation of weight-loss drugs, they pile back on the kilos four times faster than they would after ending diet and exercise regimes, new research found on Thursday.
But this was mostly because they lost so much weight in the first place, according to the British researchers who conducted the largest and most up-to-date review of the subject.
A new generation of appetite-suppressing, injectable drugs called GLP-1 agonists have become immensely popular in the last few years, transforming the treatment for obesity and diabetes in many countries.
They have been found to help people lose between 15-20 per cent of their body weight.
“This all appears to be a good news story,” said Susan Jebb, a public health nutrition scientist at Oxford University and co-author of a new BMJ study.
However, recent data has suggested that “around half of people discontinue these medications within a year”, she told a press conference.
This might be because of common side effects such as nausea or the price — these drugs can cost over $1,000 a month in the US.
So the researchers reviewed 37 studies looking at ceasing different weight-loss drugs, finding that participants regained around 0.4 kilograms a month.
Six of the clinical trials involved semaglutide — the ingredient used in Novo Nordisk’s brands Ozempic and Wegovy — and tirzepatide used for Eli Lilly’s Mounjaro and Zepbound.
While taking these two drugs, the trial participants lost an average of nearly 15 kilogrammes.
However, after stopping the medication, they regained 10 kilograms within a year, which was the longest follow-up period available for these relatively new drugs.
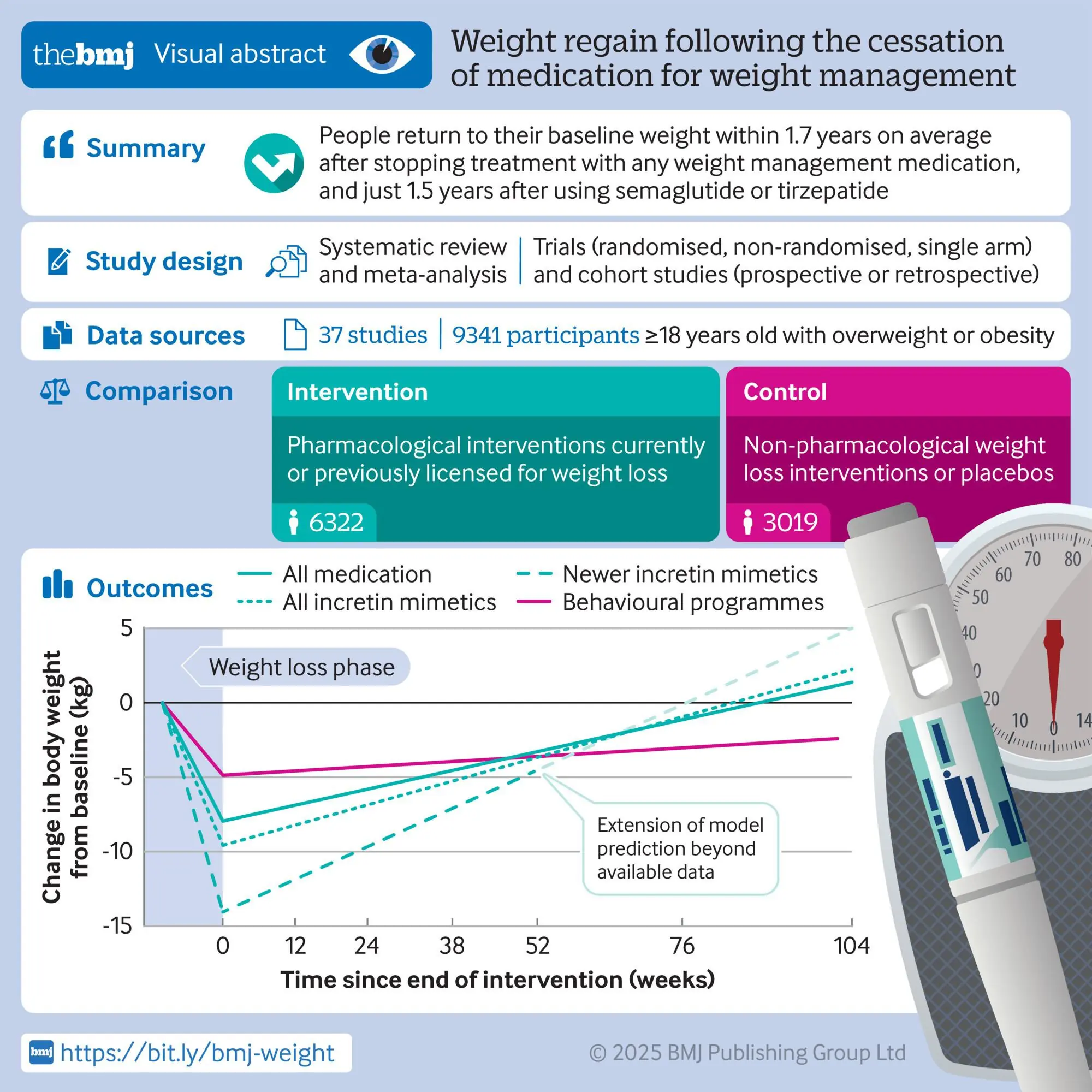
The researchers projected that the participants would return to their original weight in 18 months.
Measurements of heart health, including blood pressure and cholesterol levels, also returned to their original levels after 1.4 years.
People who were instead put on programmes that included diet and exercise — but not drugs — lost significantly less weight. However, it took an average of four years for them to regain their lost kilos.
This meant that people taking the drugs regained their weight four times faster.
‘Starting point, not a cure’
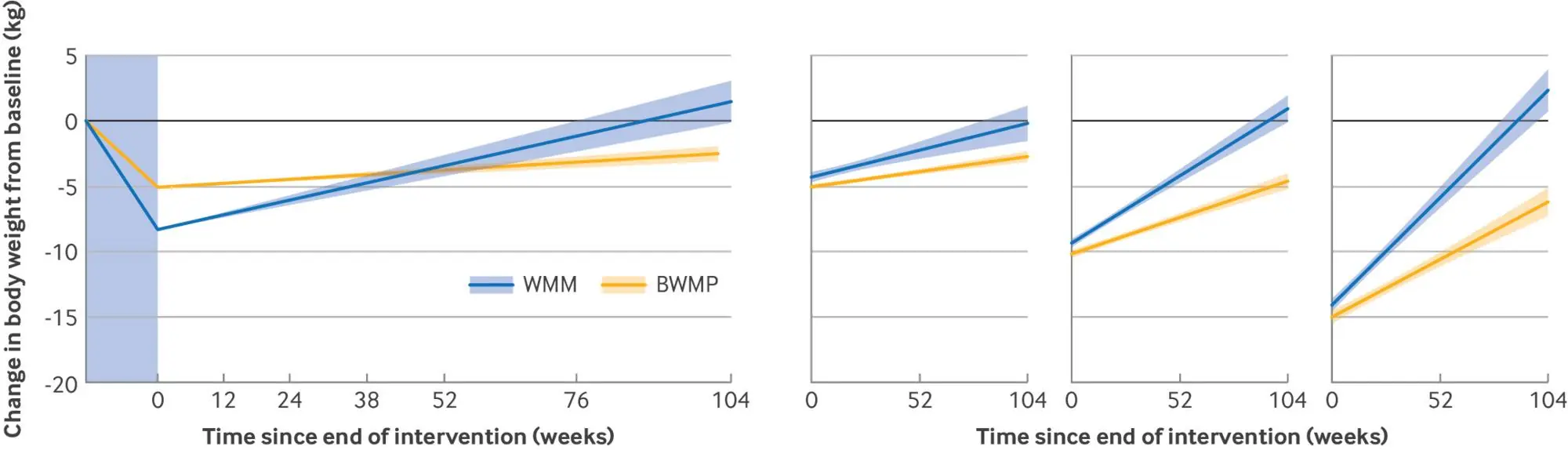
“Greater weight loss tends to result in faster weight regain,” lead study author Sam West of Oxford University explained.
But separate analysis showed that weight gain was “consistently faster after medication, regardless of the amount of weight lost in the first place,” he added.
This could be because people who have learned to eat more healthily and exercise more often continue to do so even as they regain weight.
Jebb emphasised that GLP-1 drugs “are a really valuable tool in obesity treatment — but obesity is a chronic relapsing condition”.
“One would expect that these treatments need to be continued for life, just in the same way as blood pressure medication,” Jebb said.
If this were the case, it would impact how national health systems judge whether these drugs are cost-effective, the researchers emphasised.
“This new data makes it clear they are a starting point, not a cure,” said Garron Dodd, a metabolic neuroscience researcher at the University of Melbourne, not involved in the study.
“Sustainable treatment will likely require combination approaches, longer-term strategies, and therapies that reshape how the brain interprets energy balance, not just how much people eat,” he said.