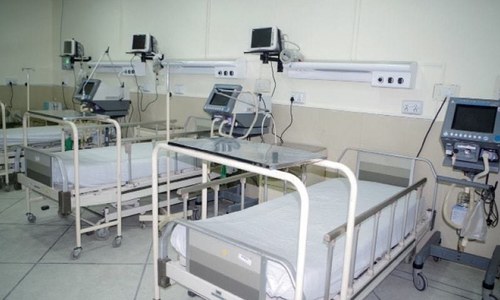
AT the end of March, Pakistan’s first ‘hero doctor’ lost his life in the fight against Covid-19. He was 26 years old. Since then, nearly 2,000 medical professionals have been infected with Covid-19; 30 of them have died. Our media is quick to portray health professionals as ‘heroes’ and ‘martyrs’, but the reality is that the pandemic is an uneven contest, testing the limits of a fragile system, exhausting existing health facilities, and consuming health workers.
Mental health: Pakistan’s Achilles heel during Covid-19
Even in normal circumstances, healthcare is a challenging profession known to adversely impact the mental health of staff, compromising their quality of life as well as work performance. And these are anything but normal circumstances. Since the pandemic began, healthcare workers’ challenges have multiplied. At a personal level, healthcare workers are afraid of contracting the virus and exposing their families to risk; burdened by the separation from their families and abdication of domestic responsibilities such as childcare; and face the social stigma that comes with working with Covid-19 patients.
Healthcare workers’ emotional needs must be addressed.
Professionally, they might feel overwhelmed by the onslaught of patients; frustrated with the lack of hospital supplies including PPEs; tired of having to make painful decisions about which patients to prioritise; exhausted from long shifts; distressed from daily conflicts at work; and distraught from having to deliver bad news to bereaved family members. These challenges are further compounded by highly tragic episodes involving doctors being arrested for demanding PPEs; having their salaries deducted for the coronavirus fund; or facing angry mobs intent on vandalising hospitals and attacking healthcare workers.
Health workers are humans too, and they need to take care of themselves so that they can continue to provide vital services during this protracted public health crisis. They routinely face conflicts over their safety being compromised as they fulfil their professional obligations. Many feel helpless dealing with an illness that has as yet no treatment. Nearly all will, at some point in this pandemic, grieve over the succumbing of their patients or colleagues to the virus. A review of six studies examining mental health issues faced by healthcare workers due to Covid-19 confirmed significant levels of distress and moderate to high levels of clinical conditions among respondents.
Despite this undeniable evidence, mental healthcare remains stigmatised in Pakistan, and the repercussions of this for those on the frontline are even more pronounced. Policymakers thus far have paid insufficient attention to the emotional needs of health workers fighting Covid-19; health managers don’t see psychosocial support as a necessity; and health workers experience shame and embarrassment in seeking help. Other countries are prioritising psychosocial support for healthcare staff, dedicating specific resources on a war footing.
The government of Pakistan has also launched a national campaign, ‘We Care’, which “aims at providing adequate PPE and creating an overall psychosocial environment of care and support”. This campaign has been verbally endorsed by provincial health ministers too.
But it is important to translate this commitment into action. A report in JAMA identified top sources of anxiety for healthcare professionals working as frontline responders and summarised their need as: Hear me (impartial mechanism to connect with health workers while maintaining confidentiality; collect data and assess their needs); Protect me (ensure personal protection, implement workplace policies to prevent burnout like adequate rest and rotation, supervise for difficult clinical decisions); Support me (workplace counselling, services for stress management, support groups, back-up support for taking time off work); Prepare me (self-help training to deal with stress, offer training to deal with psychological challenges); Care for me (identify and treat those suffering from high levels of stress and with pre-existing mental health conditions).
Implementing these strategies in Pakistan may seem far-fetched and idealistic, but similar cost-effective models already exist elsewhere and should be easy to replicate. Our provinces must prepare a comprehensive plan to support their healthcare staff on the front line. Each tertiary hospital in the country has a department of psychiatry, which in turn has at least a dozen mental health professionals. Each district hospital has at least one psychiatrist. These professionals must be assigned specific duties to support health workers in hospitals.
Health workers face both psychological and logistical barriers in seeking emotional help, not least of which is the fact that they simply don’t have the time to source support. Unless psychosocial support is immediate, effective and efficient, they will continue to suffer.
The writer is a consultant psychiatrist.
Twitter: @AsmaHumayun
Published in Dawn, June 7th, 2020